Hospital: Hospital Universitari Vall d'Hebron.
Nº: C2019-174
Aut@r o Autores: A. Aubanell, J. Arenós, P. Coscojuela, D. Hernandez, C. Vert, À. Rovira.
Presentación
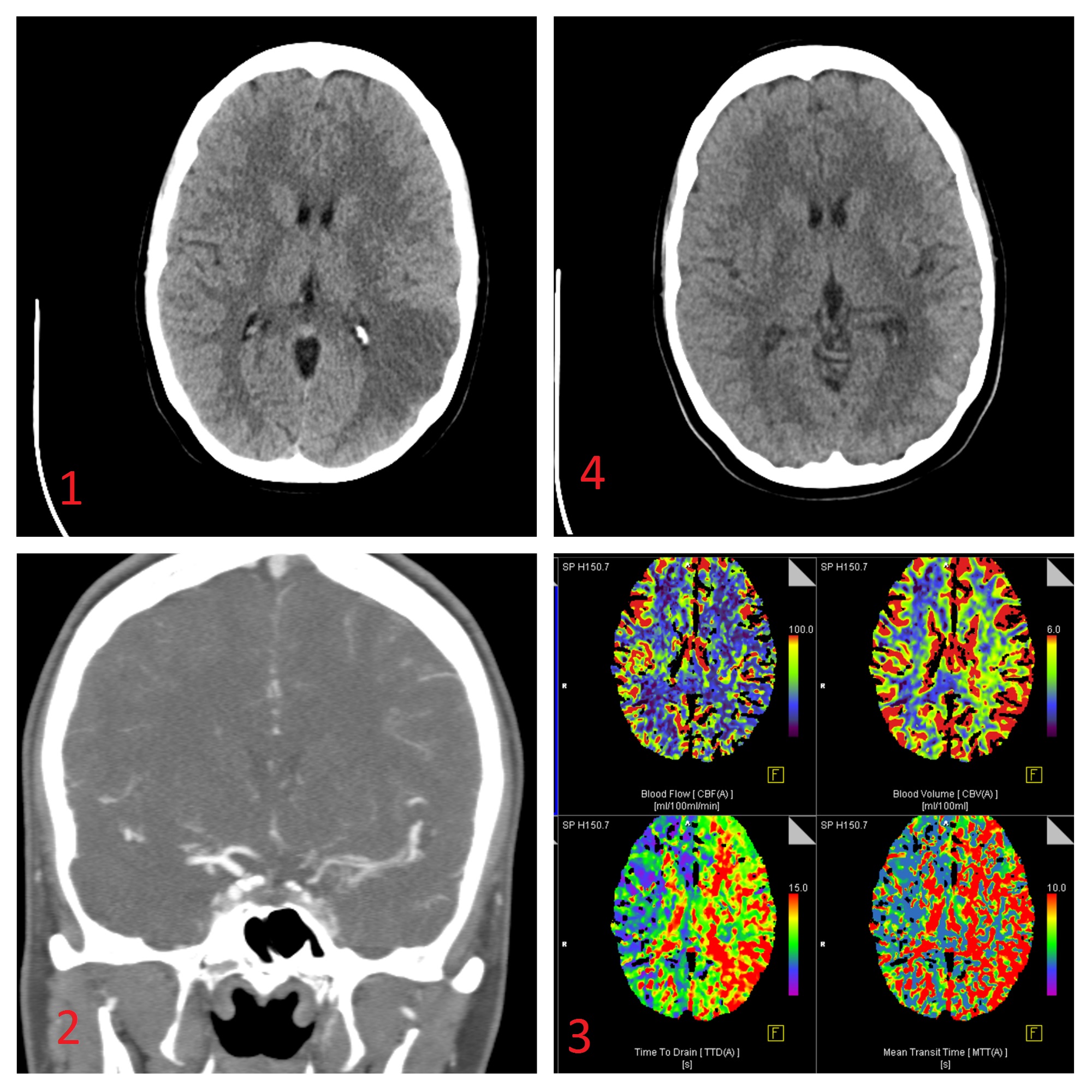
We are presenting a 23-year-old female who comes to the ER referring acute onset of hemiparesis and aphasia. She has noticed hand clumsiness during the last month with no other symptomatology or clinic antecedents. Blood test performed in the ER only showed a VSG value of 140 mm. Multimodal head CT scan was performed. In the unenhanced CT we can see a left parietal cortico-subcortical hypodensity affecting the territories of the posterior division of the left medial cerebral artery suggesting an acute ischemic event. ASPECTs score was 6/10 (Figure 1). The Angio-CT showed a pathologic left internal carotid artery. We can see a stenosis of the left internal carotid artery from the carotid bulb being more irregular in its intracranial portion with a very diminished caliber and lesion in cerebral anterior and medial arteries (Figure 2). In the perfusion-CT scan we found transit times and blood flow altered in the affected area with preservation of blood volume indicating a mismatch area. Considering this clinical and radiologic findings we reached the diagnosis of acute stroke. In order to confirm and characterize more accurately these findings a diagnostic angiography was performed (figure 3). SPECT showed no signs of vasculitis making this diagnosis less probable. Renal arteries angio-CT scan was performed showing no arterial stenosis. The patient received immunosuppressive therapy. With this treatment multimodal brain CT scan findings improved (figure 4) and surgical treatment (bypass) was dismissed. The etiology of the process is still unknown.
Discusión
This case was oriented as “Moya-Moya like syndrome” (given de blurry aspect of the angiographic study) with the following entities as a differential diagnosis: small vessel vasculitis, fibromuscular dysplasia, sickle cell disease, thrombophilia and dissection (most common cause of stroke in young people).
Conclusión
Our aim with this case is to describe the moyamoya like syndrome, the entities that can be included in the differential diagnosis and radiologic management.
Bibliografía
- Osborn AG, Hedlund GL, Salzman KL. Osbornsbrain: imaging, pathology, and anatomy. Philadelphia, PA: Elsevier, 2018. - Fujimura M, Bang OY, Kim JS. Moyamoya Disease. Front Neurol Neurosci, 2016, 40: 204-220. - Edgell RC, Boulos AS, Borhani Haghighi A, et